Agitation Reduction: Simple Ways to Calm Restlessness
Feeling restless or suddenly agitated can happen to anyone — you might feel wired, shout, pace, or struggle to focus. When agitation hits, quick, practical steps make the difference. This page gives clear, safe strategies you can use now: behavioral moves, calming breathing, environment fixes, and medication basics. Use what fits your situation and check with a doctor for ongoing or severe cases.
Recognize the trigger and the level of risk. Is the agitation mild and internal, or intense and risking harm? Mild agitation often responds to short breaks, deep breaths, or a change of scene. Severe agitation—threats, suicidal thoughts, or aggressive behavior—needs immediate professional help. If someone is dangerous to themselves or others call emergency services right away.
Start with one-minute interventions. Slow your breathing: inhale for four counts, hold one, exhale for six. Repeat five times. Ground your senses: name five things you see, four you can touch, three you hear, two you smell, one you taste. Move somewhere calmer: step outside for fresh air or sit down with a glass of water. These steps reduce adrenaline and give your brain a chance to reset.
Change the environment. Lower lights, reduce noise, and remove clutter or sharp objects. Play low-tempo music or white noise. If you care for someone who becomes agitated at predictable times, build a calm routine before those triggers. Small things—soft clothing, a weighted blanket, dimmed screens—help a lot.
Use distraction wisely. Simple tasks like folding laundry, walking slowly, or doing a short puzzle can redirect agitation. Physical activity helps release built-up energy; a brisk five-minute walk often works better than trying to force calm with stillness.
When to consider medication. Some situations need drugs: severe agitation from withdrawal, bipolar mania, psychosis, or delirium often requires short-term medication under medical supervision. Common options doctors may use include benzodiazepines for alcohol withdrawal and antipsychotics for psychosis-related agitation. Never start or stop prescription meds without a healthcare provider.
Talk and set boundaries. If someone else is agitated, use calm, short sentences. Offer choices: “Sit here or sit over there?” Avoid arguing or long explanations. For your own agitation, tell a trusted person what you need—space, a hug, or help contacting a clinician.
Longer-term strategies prevent future flare-ups. Regular sleep, steady meals, limiting caffeine and stimulants, and a basic exercise routine reduce baseline stress. Therapy techniques like CBT skills and mindfulness build long-term resilience.
If agitation is new, prolonged, or linked to mood swings, hallucinations, or self-harm, contact a healthcare provider. You deserve safety and steady support—use these hands-on tips now and reach out when you need help.
Quick toolkit
Carry a small kit: bottled water, chewing gum, a stress ball, earplugs, and a list of emergency contacts. For chronic cases, keep a written plan with preferred calming steps and medications. Share that plan with family and your doctor. Regular medication reviews and clear emergency instructions reduce panic and speed safe responses when agitation appears. Keep notes and follow up.
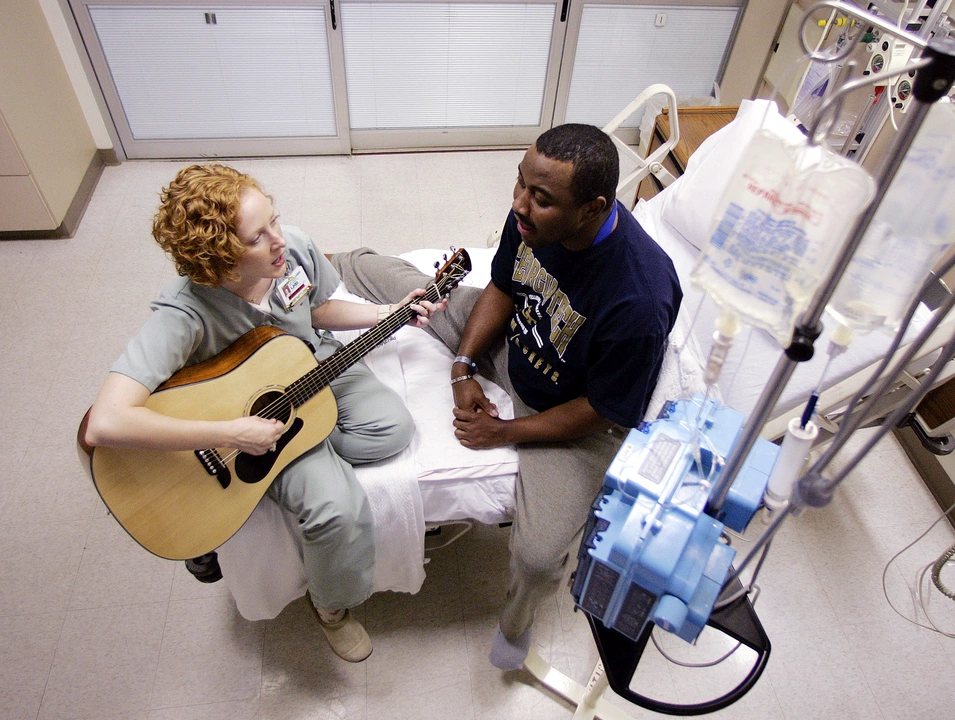
Using music therapy to alleviate agitation: a soothing approach
I recently came across an interesting approach to alleviating agitation through music therapy. It turns out that this soothing technique can be highly effective in reducing stress and promoting relaxation. By using calming and familiar tunes, music therapy helps to bring comfort and relief to those suffering from agitation. The benefits don't stop there, as it has also been shown to improve mood and overall well-being. I am truly amazed by the power of music and its potential to heal our minds and souls.
