Tamoxifen: What It Does and How to Use It
Tamoxifen is one of the most commonly used drugs for hormone receptor–positive breast cancer. It’s been around for decades and still matters because it can lower the chance of cancer returning and, in some cases, reduce the risk of developing breast cancer in the other breast.
At its core, tamoxifen blocks estrogen’s effect in breast tissue. Many breast cancers need estrogen to grow. By getting in the way, tamoxifen slows or stops that growth. Doctors prescribe it after surgery, with chemo, or alone—sometimes for five to ten years depending on the situation.
Who takes tamoxifen and how?
People with estrogen receptor–positive breast cancer are the main candidates. It’s used in premenopausal and postmenopausal women and sometimes in men with breast cancer. Typical dose is 20 mg once daily, but your doctor may adjust that. Some patients switch to different hormone drugs after menopause; others stay on tamoxifen for longer because it fits their risk profile.
Timing matters: take it around the same time every day, with or without food. Don’t stop suddenly without talking to your doctor — stopping early can raise the risk of recurrence.
Common side effects & when to call your doctor
Many people tolerate tamoxifen, but side effects happen. Hot flashes, night sweats, vaginal dryness, mood swings, and lower libido are common. Less common but important are blood clots and, rarely, uterine changes including cancer. That’s why doctors ask about any unusual vaginal bleeding, sudden leg pain or swelling, shortness of breath, severe headaches, or vision changes.
Bone health can change: tamoxifen can protect bones in premenopausal women but may affect them differently after menopause. Your care team may order bone density tests and suggest calcium, vitamin D, or other treatments if needed.
Some blood tests and pelvic exams may be scheduled during treatment. Keep all follow-up visits so issues get caught early.
Drug interactions matter. Certain antidepressants (like some SSRIs) can reduce tamoxifen’s effectiveness by blocking its conversion to the active form. Talk to your pharmacist before adding new meds, supplements, or strong herbal remedies like St. John’s wort.
Pregnancy is a no-go while taking tamoxifen. It can harm an unborn baby. Use reliable birth control and discuss timing with your doctor if you’re planning pregnancy.
Practical tips: set a daily alarm, keep pills in their original bottle, and use a single pharmacy so they can flag interactions. If side effects are rough, your doctor can often change supportive meds or suggest switching therapies.
If you’re researching options, bring a list of your other medications and a clear record of any symptoms to your next visit. Tamoxifen can be highly effective, but it works best when you and your care team stay on the same page.
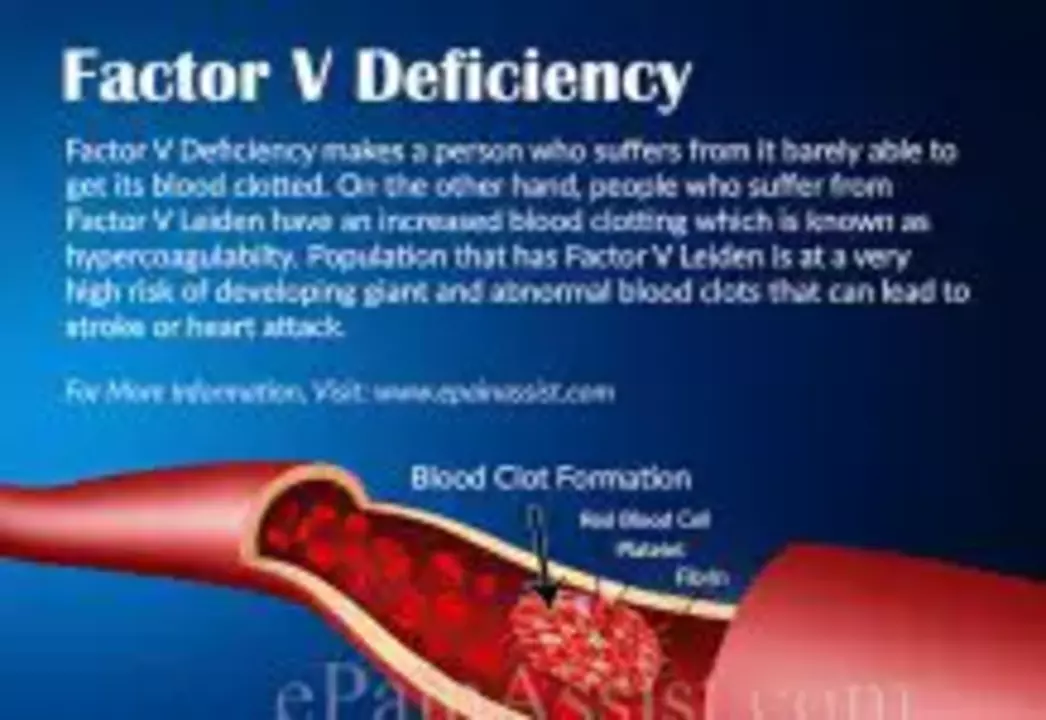
Tamoxifen and the Risk of Blood Clots: What You Need to Know
As a blogger, I recently came across some important information about Tamoxifen, a medication commonly used to treat breast cancer. One potential side effect of this drug is an increased risk of blood clots. It's crucial for patients taking Tamoxifen to be aware of this risk and monitor for any signs of blood clots, like swelling, pain, or changes in skin color. If you're on Tamoxifen, make sure to talk to your doctor about measures you can take to minimize this risk. Stay informed and proactive about your health, and don't hesitate to reach out to your healthcare provider with any concerns.
