Second-line treatment: when your first plan doesn’t work
Hearing that you need a second-line treatment can feel like a setback. But it’s often just the logical next step: your doctor switches to a different drug or approach because the first one stopped working, caused bad side effects, or isn’t the best fit. Knowing what to expect makes decisions easier and less stressful.
What second-line treatment actually is
Second-line treatment is the follow-up option after the initial (first-line) therapy fails or becomes unsafe. That can mean a different drug, a stronger dose, adding another medicine, or using a different method like surgery or radiation. For infections, it might be a different antibiotic when bacteria are resistant. For cancer, it could be a new chemo drug or targeted therapy. For chronic conditions like depression or hypertension, it often means switching drug classes.
How doctors decide and what you should ask
Doctors pick a second-line option based on why the first failed, your test results, and your overall health. Key factors include drug resistance, side effects you experienced, other conditions you have, and available evidence for the next therapy. When your doctor suggests a change, ask clear questions: Why this option? What benefits and risks should I expect? How soon should it work? Will there be extra tests or monitoring? Are there non-drug alternatives or clinical trials I should know about?
Think about practical issues too. Ask about cost, insurance coverage, and whether prior authorization is needed. If the new treatment requires more clinic visits, lab work, or special storage, get those details up front. If you take multiple medicines, request a pharmacist review to spot interactions. Bring a complete list of your drugs and supplements to appointments.
Timing matters. Some second-line treatments take days to months to show benefit. Your doctor should explain realistic timelines and what counts as improvement. If side effects show up, know who to call and when to seek urgent care. Keep a simple symptom diary for the first few weeks so you and your provider can track progress.
When to get a second opinion? If the suggested plan feels risky, unclear, or very costly, a second opinion can confirm the approach or suggest alternatives. Ask your provider for records and test results to share with another specialist. A second opinion doesn’t mean distrust—it's a smart step when the decision matters.
Don’t forget quality-of-life choices. Some second-line options prioritize longer life, others focus on comfort and fewer side effects. Talk honestly about your goals: symptom control, returning to work, or minimizing clinic visits. That helps your team tailor the plan to your life, not just the disease.
Finally, keep organized. Save treatment plans, lab results, and a list of questions. Use phone photos or a simple folder. Being proactive helps you spot problems early and makes it much easier to get the care you need if plans change again.
Want practical next steps? Write down your top concerns before the appointment, ask for clear timelines, and confirm cost and monitoring needs. That makes switching from first-line to second-line treatment a planned move, not a sudden shock.
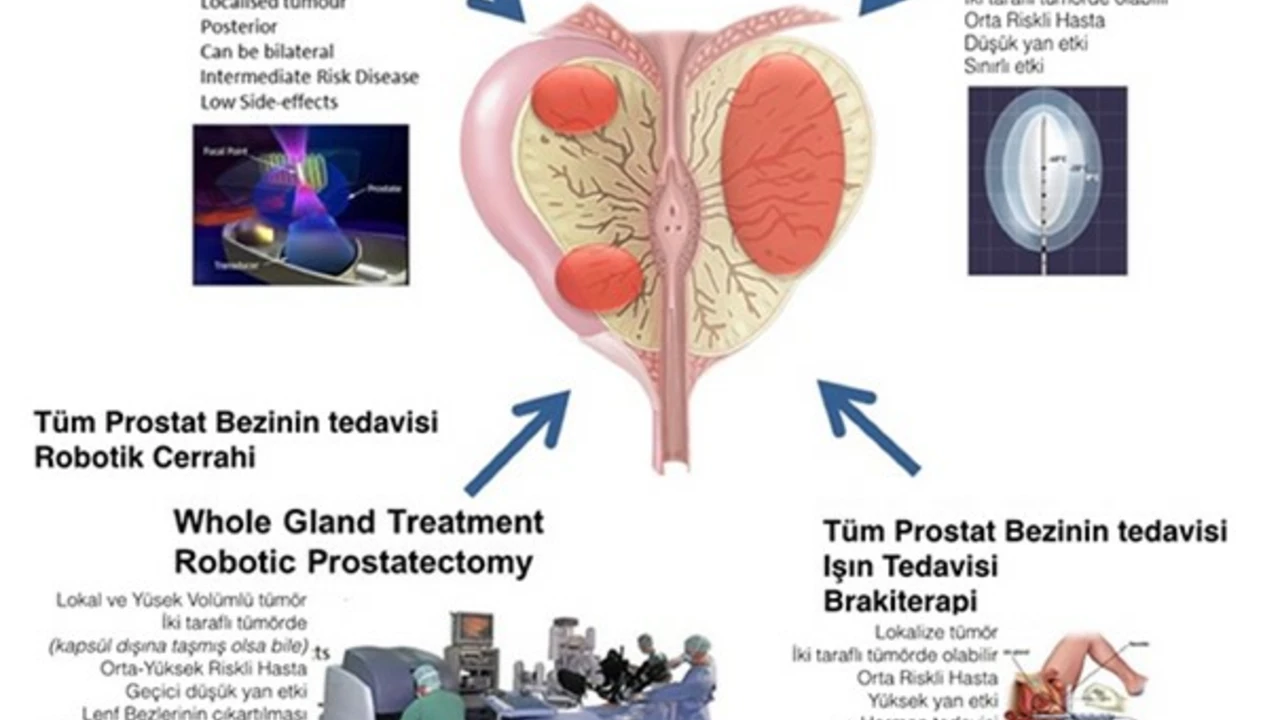
Flutamide as a Second-Line Treatment Option for Prostate Cancer
I recently delved into the topic of Flutamide as a second-line treatment for prostate cancer. Flutamide, an anti-androgen medication, is increasingly being recognized as a viable treatment option when first-line therapies fail. It works by blocking the androgen receptors, thus inhibiting the growth of cancer cells. While it does come with some side effects, the potential benefits it provides in controlling cancer progression cannot be ignored. This just goes to show the evolving nature of cancer treatments and gives hope to those battling this disease.
