Sarcoptes scabiei — how to spot and treat scabies fast
Sarcoptes scabiei is the tiny mite that causes scabies. It burrows into the top layer of skin and triggers intense itching and a rash. You don’t need medical jargon to understand it — the signs and steps to fix it are straightforward.
How to spot scabies
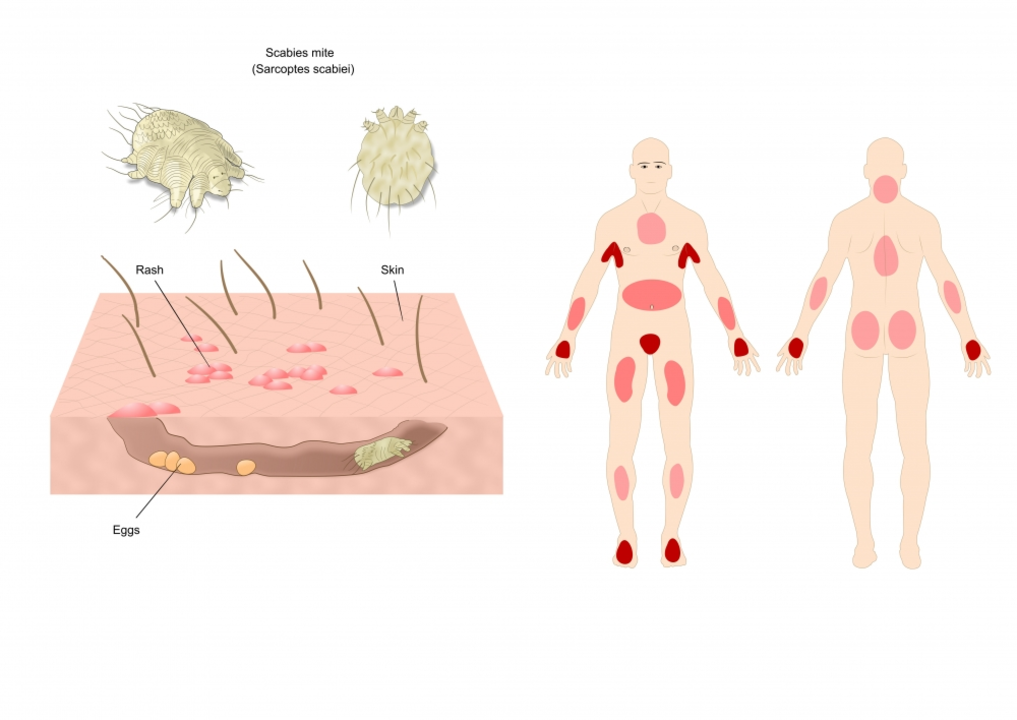
The most common symptom is itching that gets worse at night. Look for small red bumps or thin, wavy lines (burrows) most often between fingers, on wrists, around the waist, under breasts, and on the buttocks. In infants and older adults the rash can appear on the face, scalp, palms, or soles.
Scabies spreads through close skin-to-skin contact. That means sleeping in the same bed, hugging, or prolonged contact with an infected person. Shared clothing, towels, or bedding can spread it too, though direct skin contact is the main route.
If you see burrows or the pattern of itching fits, see a healthcare provider. Doctors can often diagnose by appearance alone. Sometimes they use a simple skin scrape and look under a microscope to confirm the mite or eggs.
Treatment and home care
Prescription creams and pills clear most cases. The usual first choice is a 5% permethrin cream. Apply it to the whole body from the neck down (and to the scalp in babies and elderly) and leave it on overnight — usually 8 to 14 hours. Most clinicians recommend repeating the application after one week.
Oral ivermectin is another effective option. It’s given as a single dose, usually 200 mcg/kg, and often repeated after one to two weeks. Doctors use ivermectin especially for crusted scabies, outbreaks in nursing homes, or when topical treatment isn’t practical.
Treat close contacts at the same time, even if they have no symptoms. That prevents re-infection. Wash clothing, bedding, and towels used in the last 72 hours in hot water and dry on high heat. Items that can’t be washed can be sealed in a plastic bag for 72 hours — the mites don’t survive long off a human host.
Itching can continue for weeks after successful treatment. That’s immune system reaction, not active mites. Your doctor may suggest antihistamines or a short steroid cream for relief. If you see increasing redness, pus, or fever, get checked for a bacterial skin infection — that may need antibiotics.
Special cases: crusted (Norwegian) scabies needs stronger, repeated treatment and sometimes both topical and oral therapy. Pregnant people and young infants need specific prescriptions, so talk to a clinician before using over-the-counter remedies.
Quick practical checklist: 1) See a healthcare provider to confirm. 2) Treat yourself and close contacts at the same time. 3) Wash bedding and clothes in hot water or seal them for 72 hours. 4) Expect itching to fade slowly and follow up if symptoms worsen.
Scabies is annoying but treatable. Acting fast and treating contacts and bedding cuts the risk of getting bitten again. If anything feels unusual or you don’t improve after treatment, contact your doctor for a follow-up plan.
How to prevent the spread of Sarcoptes scabiei in your home
Keeping our homes free from Sarcoptes scabiei is crucial to avoid the spread of scabies. To prevent this, we need to maintain good hygiene by washing bedding, clothes, and towels frequently in hot water. Vacuuming our home regularly, especially carpets and upholstery, helps eliminate any lingering mites. Additionally, we should avoid sharing personal items, such as clothing and bedding, with individuals who are infected. Lastly, educating ourselves and our family about the symptoms and risks of scabies can help us stay aware and proactive in preventing the spread of this contagious skin condition.
