Prostate cancer: clear answers, tests, and next steps
Prostate cancer is common in men, especially after age 50. Knowing the basics helps you spot signs early and choose the right care. This page collects practical info on symptoms, screening, tests, treatment options, and everyday steps you can take to protect prostate health.
Who gets prostate cancer and what to watch for
Older age is the biggest risk. Family history, having a father or brother with prostate cancer, raises your risk. Black men face higher rates and often more aggressive disease. Early prostate cancer may not cause symptoms. When symptoms appear they often include weak urine flow, needing to urinate more at night, difficulty starting, blood in urine or semen, or new pelvic discomfort. These signs can come from other conditions such as benign prostatic hyperplasia or infection, but talk to a doctor if you notice them.
Screening and diagnosis: PSA, exam, and biopsy
Screening usually starts with a PSA blood test and a digital rectal exam (DRE). A single elevated PSA doesn’t mean cancer. Your doctor may repeat the test, check for infections, or use free/total PSA ratios. If results look concerning, MRI and a prostate biopsy can confirm the diagnosis. MRI-guided biopsies are more accurate and reduce unnecessary sampling. Ask your doctor about risks and what the results mean for your situation.
Treatment options explained simply
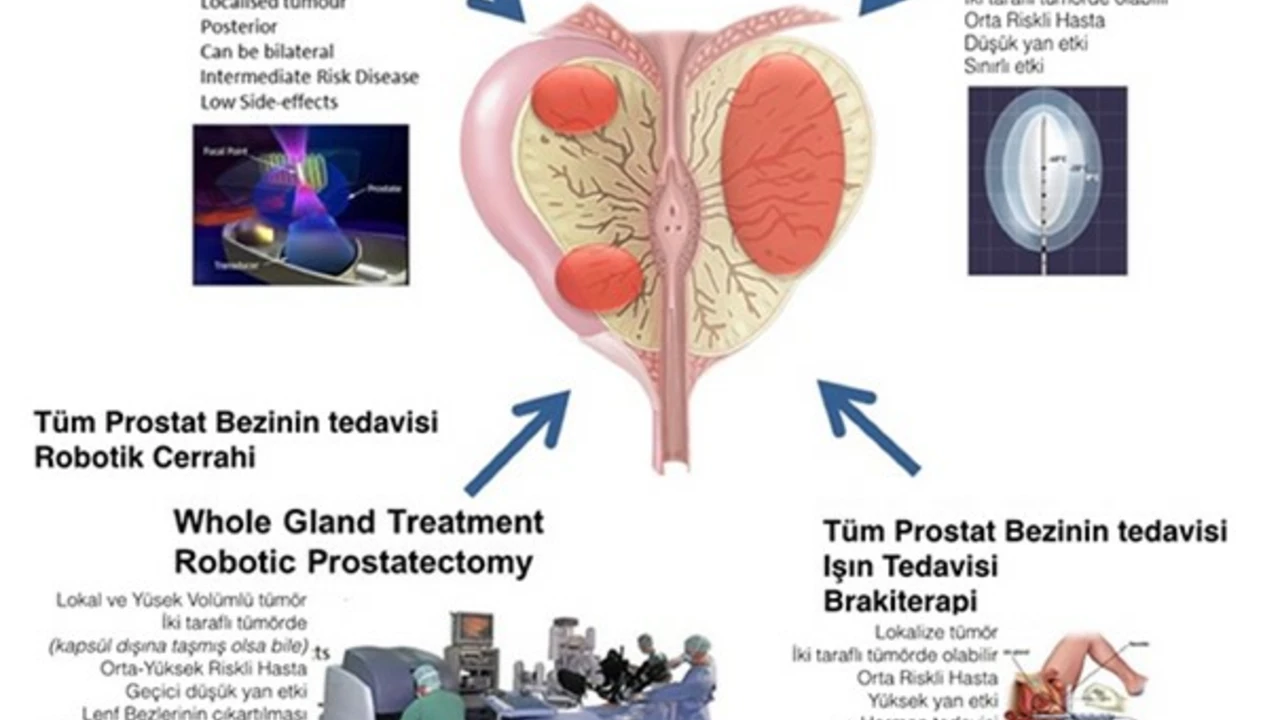
Treatment depends on cancer grade, stage, age, and health. For low-risk tumors, active surveillance means regular PSA checks and biopsies instead of immediate treatment. For localized cancer, surgery (prostatectomy) or radiation can remove or destroy the tumor. Side effects include urinary leakage and sexual changes; talk honestly with your care team about risks and recovery plans. Advanced or metastatic prostate cancer often needs hormone therapy to lower testosterone, sometimes combined with chemotherapy or newer targeted drugs. Clinical trials can offer access to new treatments; ask if any fit your case.
Daily steps that help
You can’t prevent all prostate cancer, but healthy habits lower risk and aid recovery. Stay active—30 minutes most days helps. Eat more vegetables, lean proteins, and reduce processed meats. Maintain a healthy weight and don’t smoke. If you’re on treatment, pelvic floor exercises can reduce leakage and improve recovery after surgery or radiation.
Deciding and asking the right questions
Bring a list to appointments: What grade and stage is my cancer? What are the treatment goals? What are likely side effects and recovery timelines? Would a second opinion help? Consider support groups and counseling—cancer affects partners and family too.
Where to learn more
Trust national cancer sites, university hospitals, and your treating oncologist for tailored info. If you need help finding specialists or clinical trials, ask your primary doctor or use reputable online registries.
If you get a diagnosis, take time to learn about Gleason score and stage—these tell how fast the cancer might grow. Get test copies, ask for treatment timelines, and discuss quality-of-life issues like sexual function and continence before deciding. Small steps now can make later choices easier. Bring a partner or friend along.
Flutamide as a Second-Line Treatment Option for Prostate Cancer
I recently delved into the topic of Flutamide as a second-line treatment for prostate cancer. Flutamide, an anti-androgen medication, is increasingly being recognized as a viable treatment option when first-line therapies fail. It works by blocking the androgen receptors, thus inhibiting the growth of cancer cells. While it does come with some side effects, the potential benefits it provides in controlling cancer progression cannot be ignored. This just goes to show the evolving nature of cancer treatments and gives hope to those battling this disease.
